Psoriatic Arthritis (PsA)
What is Psoriatic Arthritis (PsA)?
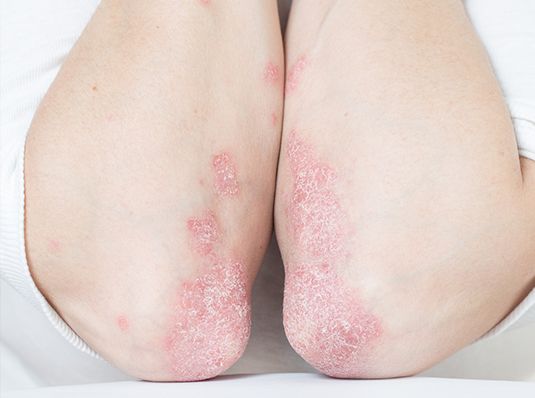
Psoriatic arthritis (PsA) is a condition that combines the swollen, sore joints of arthritis with psoriasis. Psoriasis causes itchy, scaly red patches to appear on your skin and scalp.
Why You Should Care:
About 7.5 million Americans have psoriasis and up to 30 percent of these people develop PsA.
Types of psoriatic arthritis:
- Symmetric PsA: This type affects the same joints on both sides of your body. About 50 percent of people with PsA have this type.
- Asymmetric PsA: This affects a joint or joints on one side of your body. It affects about 35 percent of people with PsA.
- Distal interphalangeal predominant PsA: This type involves the joints closest to your nails. It occurs in about 10 percent of people with PsA.
- Spondylitis PsA: This type of PsA involves your spine. Your entire spine from your neck to your lower back may be affected.
- Psoriatic arthritis mutilans: About 5 percent of people with PsA have this type. Psoriatic arthritis mutilans usually affects your hands and feet.
Symptoms:
General symptoms of PsA include:
- Swollen, tender joints on one or both sides of your body
- Morning stiffness
- Swollen fingers and toes
- Painful muscles and tendons
- Scaly skin patches, which may get worse when joint pain flares up
- Flaky scalp
- Fatigue
- Nail Pitting
- Separation of your nail from the nail bed
- Eye redness (conjunctivitis)
- Eye pain (uveitis)
Spondylitis PsA, in particular, can also cause the following symptoms:
- Spinal pain and stiffness
- Pain, swelling, and weakness in your hips, knees, ankles, feet, elbow, hands, wrists, and other joints
- Swollen toes or fingers
Risk Factors:
You’re more likely to get PsA if you:
- Have psoriasis
- Have a parent, brother, or sister with PsA
- Are between the ages of 30 and 50 (though children can get it, too)
- Have had strep throat
- Have HIV
PsA puts you at risk for complications that include:
- Psoriatic arthritis mutilans
- Eye problems, such as conjunctivitis or uveitis
- Cardiovascular disease
Psoriatic Arthritis Triggers:
PsA flare-ups make the condition worse for a period of time. Certain things can set off PsA flares and these things are different for everybody.
Common PsA triggers include:
- Infections like strep throat and upper respiratory infection
- Injuries such as a cut, scrape, or sunburn
- Dry skin
- Stress
- Cold, dry weather
- Smoking
- Heavy drinking
- Excess weight
- Medicines such as lithium, beta-blockers, and antimalarial drugs
Although you can’t avoid all of these triggers, you can try to manage stress, stop smoking, and cut down on drinking.
Treatment:
The goal of PsA treatment is to improve symptoms like skin rash and joint inflammation. A typical treatment plan will include one or more of the following:
- Nonsteroidal anti-inflammatory drugs (NSAIDs): These medications help control joint pain and swelling. Over-the-counter (OTC) options include ibuprofen (Advil) and naproxen (Aleve).
- Disease-modifying antirheumatic drugs (DMARDs): These medications decrease inflammation to prevent joint damage and slow the progression of PsA. The most commonly prescribed DMARDs include:
- Methotrexate (Trexall)
- Leflunomide (Arava)
- Sulfasalazine (Azulfidine)
- Apremilast (Otezla)
- Biologics: Commonly prescribed biologic drugs include:
- Adalimumab (Humira)
- Certolizumab (Cimzia)
- Golimumab (Simponi)
- Etanercept (Enbrel)
- Infliximab (Remicade)
- Steroids: These medications can bring down inflammation. For PsA, they’re usually injected into affected joints.
- Immunosuppressants: Medications like azathioprine (Imuran) and cyclosporine (Gengraf) calm the overactive immune response in PsA.
- Biologics: Commonly prescribed biologic drugs include:
- Topical treatments: Creams, gels, lotions, and ointments can relieve the itchy PsA rash. Options include:
- Anthralin
- Calcitriol or Calcipotriene, which are forms of vitamin D-3
- Salicylic Acid
- Steroid Creams
- Tazarotene, which is a derivative of vitamin AA
- Light therapy and other PsA medicines: Light therapy uses medicine, followed by exposure to bright light, to treat psoriasis skin rashes.
CIS does not provide medical advice, diagnosis or treatment. The content provided is for informational purposes only.
Back To Health Education